INTRODUCTIONS
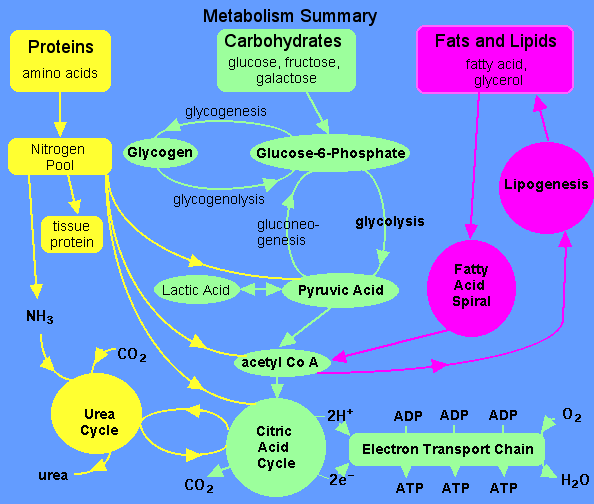
Carbohydrate metabolism begins with digestion in the small intestine where monosaccharides are absorbed into the blood stream. Blood sugar concentrations are controlled by three hormones: insulin, glucagon, and epinephrine. If the concentration of glucose in the blood is too high, insulin is secreted by the pancreas. Insulin stimulates the transfer of glucose into the cells, especially in the liver and muscles, although other organs are also able to metabolize glucose.
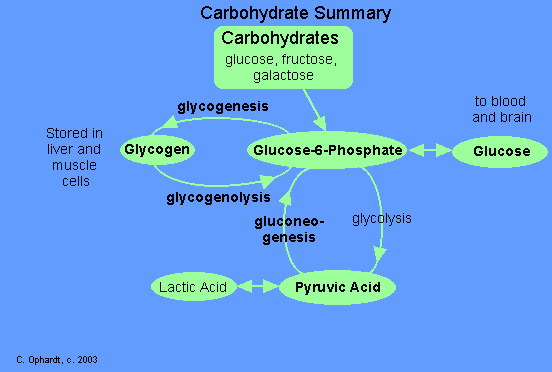
In the liver and muscles, most of the glucose is changed into glycogen by the process of glycogenesis (anabolism). Glycogen is stored in the liver and muscles until needed at some later time when glucose levels are low. If blood glucose levels are low, then eqinephrine and glucogon hormones are secreted to stimulate the conversion of glycogen to glucose. This process is called glycogenolysis (catabolism).
If glucose is needed immediately upon entering the cells to supply energy, it begins the metabolic process called glycoysis (catabolism). The end products of glycolysis are pyruvic acid and ATP.
Since glycolysis releases relatively little ATP, further reactions continue to convert pyruvic acid to acetyl CoA and then citric acid in the citric acid cycle. The majority of the ATP is made from oxidations in the citric acid cycle in connection with the electron transport chain.
During strenuous muscular activity, pyruvic acid is converted into lactic acid rather thatn acetyl CoA. Durlng the resting period, the lactic acid is converted back to pyruvic acid. The pyruvic acid in turn is converted back to glucose by the process called gluconeogenesis (anabolism). If the glucose is not needed at that moment, it is converted into glycogen by glycogenesis. You can remember those terms if you think of "genesis" as the formation-beginning.
Glycogenesis, Glycogenolysis and Gluconeogenesis
Biosynthesis of Glycogen
The goal of glycolysis, glycogenolysis, and the citric acid cycle is to conserve energy as ATP from the catabolism of carbohydrates. If the cells have sufficient supplies of ATP, then these pathways and cycles are inhibited. Under these conditions of excess ATP, the liver will attempt to convert a variety of excess molecules into glucose and/or glycogen.
Glycogenesis
Glycogenesis is the formation of glycogen fromglucose. Glycogen is synthesized depending on the demand for glucose and ATP (energy). If both are present in relatively high amounts, then the excess of insulin promotes the glucose conversion into glycogen for storage in liver and muscle cells.
In the synthesis of glycogen, one ATP is required per glucose incorporated into the polymeric branched structure of glycogen. actually, glucose-6-phosphate is the cross-roads compound. Glucose-6-phosphate is synthesized directly from glucose or as the end product of gluconeogenesis.
Glycogenesis is the formation of glycogen fromglucose. Glycogen is synthesized depending on the demand for glucose and ATP (energy). If both are present in relatively high amounts, then the excess of insulin promotes the glucose conversion into glycogen for storage in liver and muscle cells.
In the synthesis of glycogen, one ATP is required per glucose incorporated into the polymeric branched structure of glycogen. actually, glucose-6-phosphate is the cross-roads compound. Glucose-6-phosphate is synthesized directly from glucose or as the end product of gluconeogenesis.
Glycogenolysis:
In glycogenolysis, glycogen stored in the liver and muscles, is converted first to glucose-1- phosphate and then into glucose-6-phosphate. Two hormones which control glycogenolysis are a peptide, glucagon from the pancreas and epinephrine from the adrenal glands.
Glucagon is released from the pancreas in response to low blood glucose and epinephrine is released in response to a threat or stress. Both hormones act upon enzymes to stimulate glycogen phosphorylase to begin glycogenolysis and inhibit glycogen synthetase (to stop glycogenesis).
Glycogen is a highly branched polymeric structure containing glucose as the basic monomer. First individual glucose molecules are hydrolyzed from the chain, followed by the addition of a phosphate group at C-1. In the next step the phosphate is moved to the C-6 position to give glucose 6-phosphate, a cross road compound.
Glucose-6-phosphate is the first step of the glycolysis pathway if glycogen is the carbohydrate source and further energy is needed. If energy is not immediately needed, the glucose-6-phosphate is converted to glucose for distribution in the blood to various cells such as brain cells.
Gluconeogenesis:
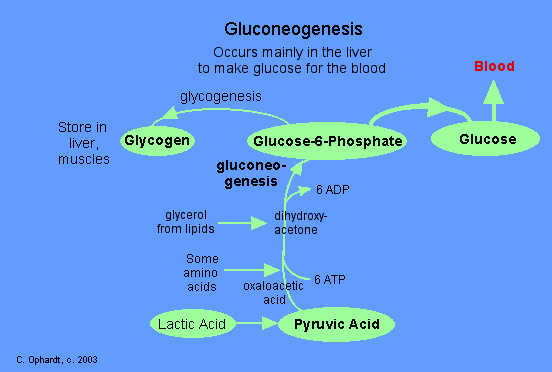
Gluconeogenesis is the process of synthesizing glucose from non-carbohydrate sources. The starting point of gluconeogenesis is pyruvic acid, although oxaloacetic acid and dihydroxyacetone phosphate also provide entry points. Lactic acid, some amino acids from protein and glycerol from fat can be converted into glucose. Gluconeogenesis is similar but not the exact reverse of glycolysis, some of the steps are the identical in reverse direction and three of them are new ones. Without going into detail, the general gluconeogenesis sequence is given in the graphic on the left.
Notice that oxaloacetic acid is synthesized from pyruvic acid in the first step. Oxaloacetic acid is also the first compound to react with acetyl CoA in the citric acid cycle. The concentration of acetyl CoA and ATP determines the fate of oxaloacetic acid. If the concentration of acetyl CoA is low and concentration of ATP is high then gluconeogenesis proceeds. Also notice that ATP is required for a biosynthesis sequence of gluconeogenesis.
Gluconeogenesis occurs mainly in the liver with a small amount also occurring in the cortex of the kidney. Very little gluconeogenesis occurs in the brain, skeletal muscles, heart muscles or other body tissue. In fact, these organs have a high demand for glucose. Therefore, gluconeogenesis is constantly occurring in the liver to maintain the glucose level in the blood to meet these demands.